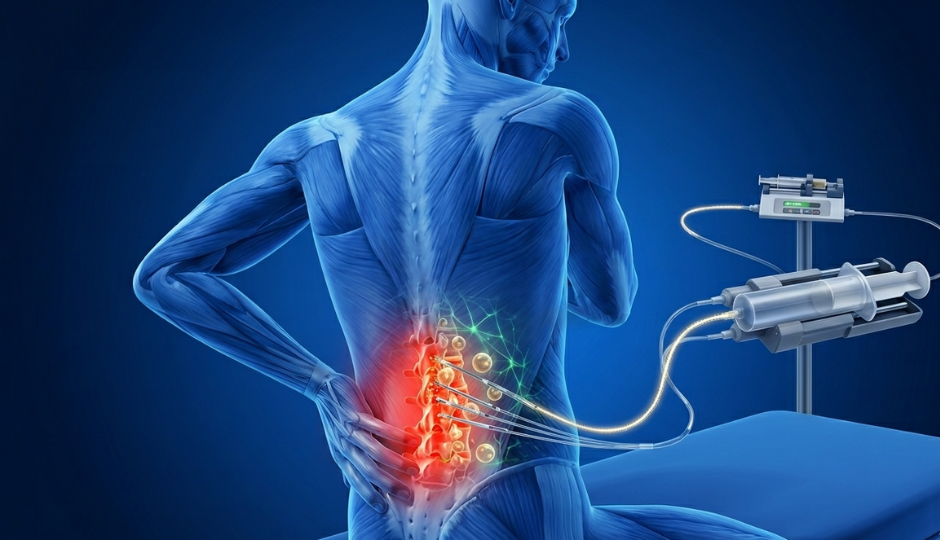
The spinal cord is the main communication pathway between the brain and the rest of the body. When it is damaged by trauma, compression, or vascular injury, the signals that control movement, sensation, and autonomic function are disrupted at the injury site and below.
Spinal cord injuries are classified by the American Spinal Injury Association (ASIA) scale from A to E, ranging from complete injury with no motor or sensory function below the level of injury to incomplete injuries where partial function is preserved. The distinction between complete and incomplete injuries matters clinically; incomplete injuries carry a better prognosis for recovery, including with regenerative approaches.
The long-term consequences of spinal cord injury depend on the level and completeness of the injury, but commonly include:
- Paralysis or paresis: Complete or partial loss of voluntary movement below the level of injury, affecting limbs, trunk, and fine motor function depending on the injury level
- Sensory loss: Reduced or absent sensation of touch, temperature, pain, and proprioception below the injury site
- Bladder and bowel dysfunction: Loss of voluntary control, requiring management strategies that significantly affect daily life
- Spasticity: involuntary muscle stiffness and spasms below the injury level, often painful and limiting to function
- Chronic neuropathic pain: Persistent burning, stabbing, or pressure pain generated by damaged neural circuits, present in a significant proportion of SCI patients
- Respiratory complications: In cervical and high thoracic injuries, impaired breathing muscle function requires ventilatory support
- Autonomic dysreflexia: Dangerous episodes of uncontrolled blood pressure in injuries above T6, triggered by stimuli below the injury level
- Psychological impact: Depression, anxiety, and adjustment difficulties are common and compound the physical challenges of living with SCI
Secondary injury, the ongoing biological damage that occurs in the hours, days, and weeks after the initial trauma, is a critical concept in SCI management. Inflammation, oxidative stress, excitotoxicity, and cell death in the surrounding tissue persist long after the injury, and this secondary cascade is responsible for a significant proportion of the final neurological deficit.