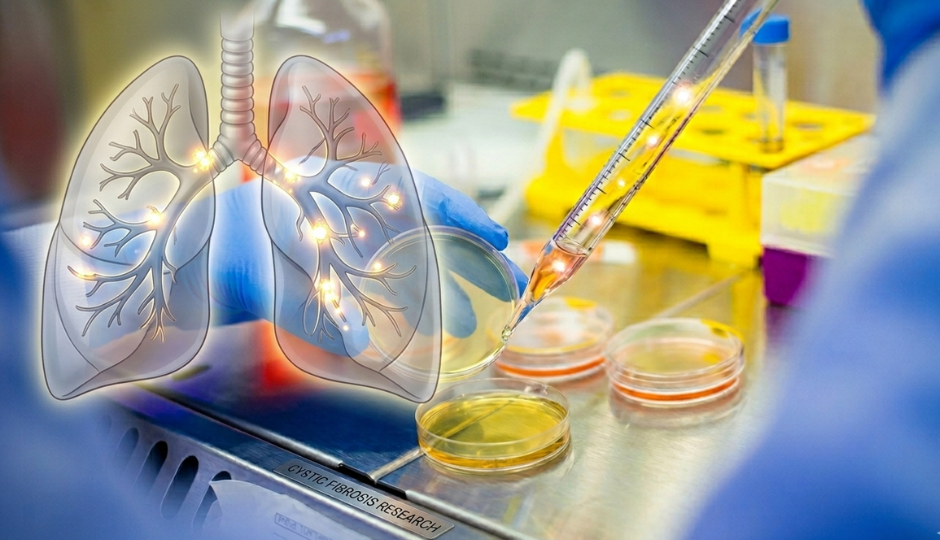
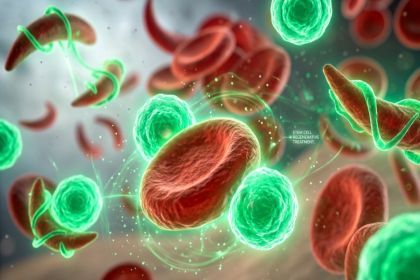
Cystic fibrosis is caused by mutations in the CFTR gene, which encodes a protein that regulates the transport of chloride and sodium ions across cell membranes. When this protein is absent or dysfunctional, the result is thick, sticky mucus that accumulates in the lungs, digestive system, liver, and other organs.
More than 2,000 CFTR mutations have been identified, though a relatively small number account for the majority of cases. The F508del mutation, the most common CF mutation globally, accounts for approximately 70% of CF alleles worldwide, according to the Cystic Fibrosis Mutation Database.
The consequences of CFTR dysfunction extend well beyond mucus accumulation:
- Chronic pulmonary infection: Thick mucus creates an ideal environment for bacterial colonisation, particularly by Pseudomonas aeruginosa and Staphylococcus aureus. Chronic infection becomes established in most CF patients during childhood and drives progressive lung damage
- Bronchiectasis: permanent structural widening and scarring of the airways resulting from repeated cycles of infection and inflammation. According to a study published in the European Respiratory Journal, bronchiectasis is present in the majority of CF patients by early adulthood and is a primary driver of lung function decline
- Pancreatic insufficiency: CFTR dysfunction impairs pancreatic enzyme secretion in approximately 85–90% of CF patients, leading to malabsorption, malnutrition, and CF-related diabetes
- Liver disease: Biliary obstruction and progressive liver fibrosis affect a significant minority of CF patients, with CF-related liver disease being a leading cause of non-pulmonary mortality
- Chronic sinusitis: Persistent sinus infection and inflammation affecting quality of life and acting as a bacterial reservoir
- Bone disease: Reduced bone mineral density is common in CF due to malabsorption, chronic inflammation, and corticosteroid use, increasing fracture risk
- Fertility complications: The majority of males with CF are infertile due to congenital absence of the vas deferens
The median predicted survival age for CF patients has improved substantially, from under 30 years in the 1990s to over 50 years in high-income countries with access to modern treatment, according to the Cystic Fibrosis Foundation Patient Registry. However, this improvement is uneven, and a significant proportion of patients continue to experience rapid progression despite optimal conventional care.