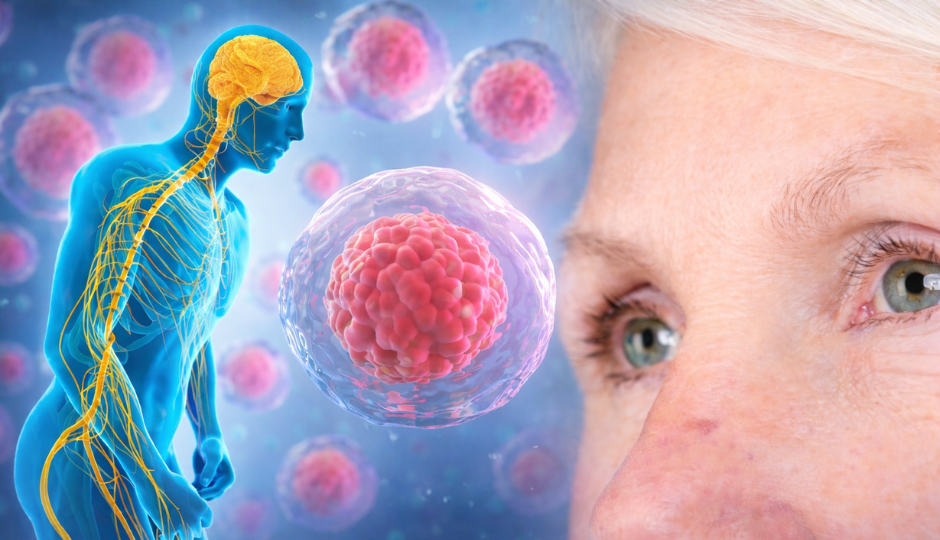
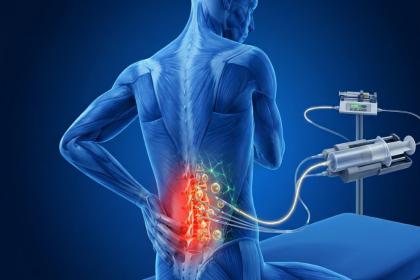
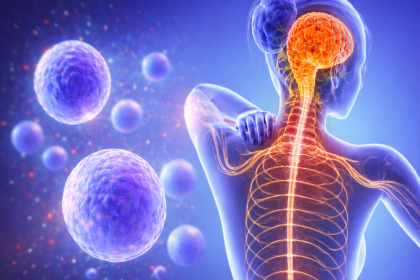
Parkinson's disease is a progressive neurodegenerative condition caused by the loss of dopaminergic neurons in the substantia nigra, a region of the brain responsible for coordinating smooth, controlled movement. As these cells die, dopamine levels fall, and the brain's ability to regulate motor function becomes increasingly compromised.
The condition is more than a movement disorder. Parkinson's affects multiple systems, autonomic, cognitive, and psychiatric, and its non-motor features are often as disabling as its physical ones. How quickly it progresses differs between people, but the direction does not.
Common long-term consequences of Parkinson's disease include:
- Tremor: Typically, a resting tremor affecting the hands, arms, legs, jaw, or face; one of the most recognisable features of the condition
- Bradykinesia: Slowness of movement that affects walking speed, facial expression, handwriting, and the ability to perform rapid, repetitive tasks
- Rigidity: Muscle stiffness causing reduced range of motion, pain, and a characteristic shuffling gait
- Postural instability: Impaired balance and righting reflexes, increasing the risk of falls
- Freezing of gait: Sudden, involuntary episodes where the feet feel fixed to the ground
- Cognitive decline: Ranging from mild cognitive impairment to Parkinson's dementia in more advanced disease
- Autonomic dysfunction: Including constipation, urinary urgency, orthostatic hypotension, and excessive sweating
- Sleep disturbances: REM sleep behaviour disorder, insomnia, and excessive daytime sleepiness
- Depression and anxiety: Affecting the majority of patients at some point during the course of the disease
- Dyskinesias: Involuntary movements that develop as a complication of long-term levodopa therapy
These consequences accumulate over time. For many patients and families, that combination, a condition that progresses regardless, and treatments that manage rather than modify, is a difficult thing to sit with.