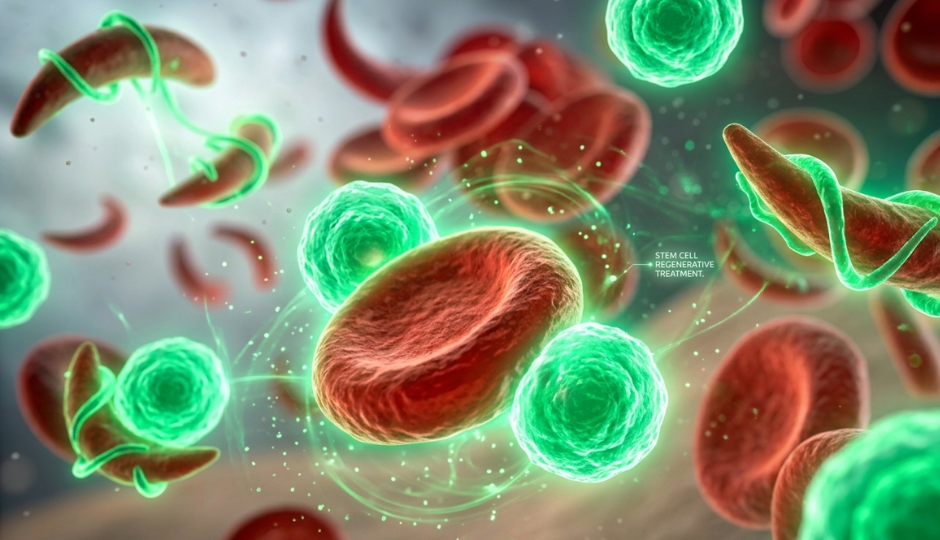
Sickle cell disease (SCD) is an inherited blood disorder caused by a mutation in the gene that encodes haemoglobin, the protein in red blood cells that carries oxygen. In SCD, this mutation produces an abnormal form called haemoglobin S. When haemoglobin S releases oxygen, it causes red blood cells to change shape, from the normal flexible disc into a rigid, crescent or sickle shape.
These sickle-shaped cells cause problems in two main ways. First, they are fragile and break down much faster than normal red blood cells, leading to chronic anaemia. Second, their rigid shape causes them to clump together and block small blood vessels, cutting off oxygen supply to tissues and organs. This is what causes a vaso-occlusive crisis, the episodes of severe pain that are the most recognisable feature of the condition.
SCD affects approximately 300,000 newborns globally each year, according to the reports of the World Health Organisation.
Long-term complications of sickle cell disease include:
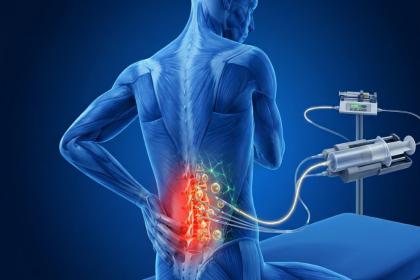
- Vaso-occlusive crises: Episodes of intense pain caused by blocked blood vessels, most commonly affecting the chest, abdomen, joints, and bones
- Acute chest syndrome: A serious lung complication that is a leading cause of hospitalisation and death in SCD patients
- Stroke: Children with SCD are approximately 300 times more likely to have a stroke than their healthy peers, according to published research
- Chronic organ damage: The kidneys, liver, spleen, and heart are all vulnerable to cumulative damage from repeated vaso-occlusive episodes
- Avascular necrosis: Death of bone tissue due to impaired blood supply, most commonly affecting the hip and shoulder
- Chronic anaemia: Persistent low red blood cell count causing fatigue, reduced exercise tolerance, and impaired cognitive function
- Pulmonary hypertension: Elevated blood pressure in the lungs, a serious long-term complication in adult SCD patients