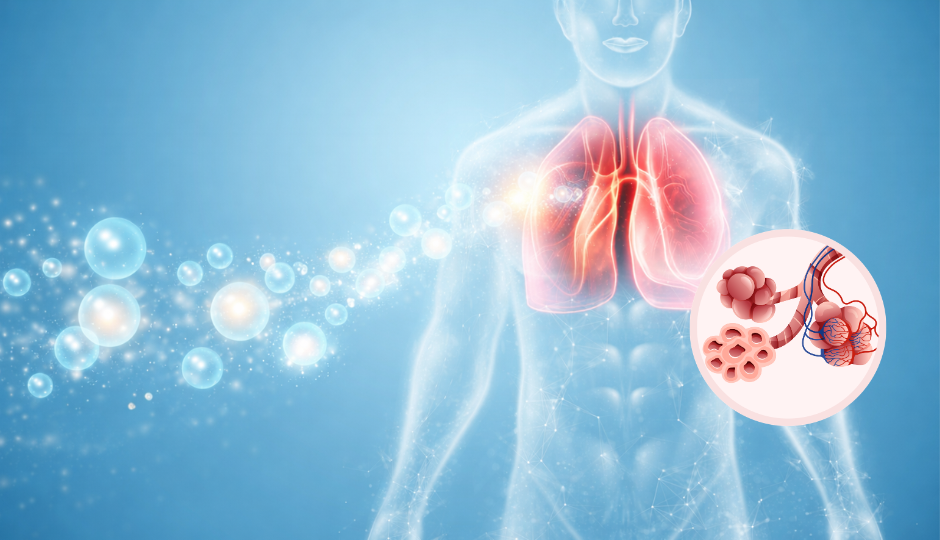
Pulmonary fibrosis describes a group of lung conditions characterised by the progressive scarring of lung parenchyma, the functional tissue responsible for gas exchange. In idiopathic pulmonary fibrosis, this scarring occurs without an identifiable external cause. In other forms, it may follow autoimmune disease (such as rheumatoid arthritis or systemic sclerosis), prolonged exposure to dust or environmental toxins, medication toxicity, or prior infection, including viral pneumonia.
The trigger differs between patients, but what follows is broadly similar: chronic injury to the delicate air sacs (alveoli) triggers an abnormal repair response, laying down collagen and fibrous tissue where healthy, elastic lung tissue once existed. The lung's capacity to expand and exchange gases diminishes over time.
Common long-term consequences of pulmonary fibrosis include:
- Progressive breathlessness - initially on exertion, later at rest as the condition advances
- Persistent dry cough - often distressing and difficult to control
- Reduced exercise tolerance - limiting mobility and independence
- Chronic fatigue - driven by reduced oxygen delivery and the effort of breathing
- Hypoxaemia - low blood oxygen levels, requiring supplemental oxygen in many patients
- Clubbing of the fingers - a physical sign of chronic oxygen deficiency
- Pulmonary hypertension - elevated blood pressure in the lung arteries, complicating the disease in advanced stages
- Acute exacerbations - sudden, sometimes severe worsening of symptoms that can be life-threatening
The psychological burden is also substantial. Anxiety, depression, and social withdrawal are common in patients living with a condition that is both unpredictable and progressive.