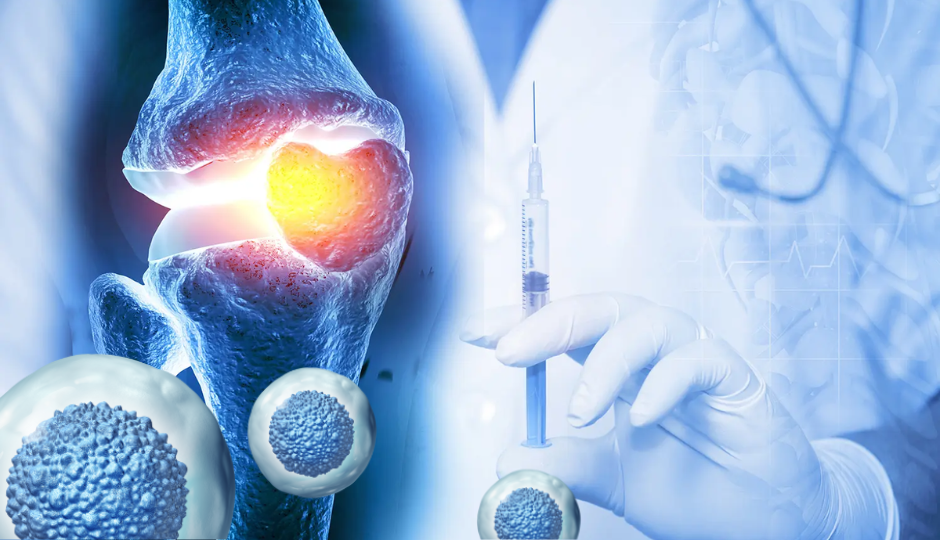
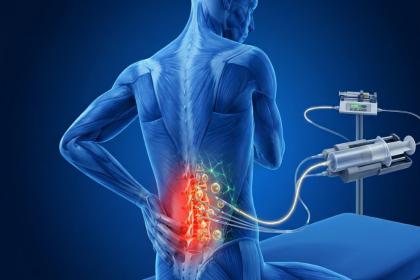
Osteoarthritis is the most common joint condition worldwide. It occurs when the cartilage that cushions the ends of bones within a joint gradually breaks down, leading to pain, stiffness, and reduced range of motion. As cartilage wears away, bones begin to rub against each other, a process that further inflames the joint and accelerates joint damage.
It most commonly affects the knees, hips, hands, and spine, though any joint can be involved. The condition is progressive. Without intervention that addresses the underlying deterioration, it tends to worsen over time.
Common long-term consequences of osteoarthritis include:
- Chronic joint pain: Ranging from a persistent dull ache to sharp pain with movement, often worsening with activity and towards the end of the day.
- Morning stiffness: Joints that feel locked or stiff on waking, typically lasting 30 minutes or less.
- Reduced range of motion: Gradual loss of the joint's ability to move through its full arc, affecting everyday tasks.
- Joint swelling: Accumulation of fluid in the joint in response to inflammation.
- Muscle weakness: Surrounding muscles weaken when a painful joint is used less, creating a cycle that accelerates decline.
- Bone spurs (osteophytes): Bony outgrowths that develop around damaged joints, contributing to pain and restricted movement
- Impact on daily function: Difficulty walking, climbing stairs, gripping objects, and performing tasks that were previously unremarkable.
These changes accumulate over the years and can significantly limit independence and quality of life. Many patients reach a point where pain is constant, sleep is disrupted, and the prospect of major joint replacement surgery feels both necessary and daunting.