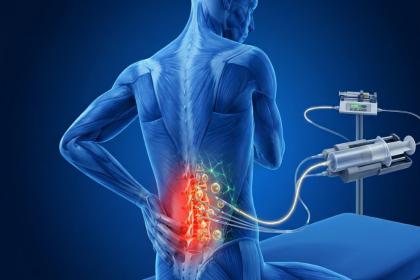
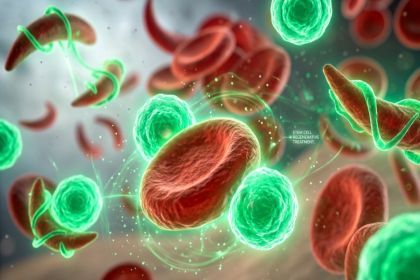
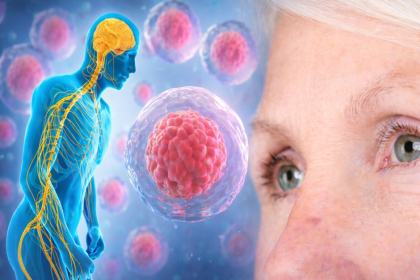
The immune system normally distinguishes between the body's own cells and foreign invaders. In autoimmune conditions, that distinction breaks down. The immune system begins producing antibodies and inflammatory signals directed at healthy tissues, and in many cases, it does not stop.
There are over 80 recognised autoimmune conditions. They vary enormously in which tissues they target and how they progress, but several biological features appear consistently across the spectrum:
- Chronic immune dysregulation: An overactive or misdirected immune response that sustains ongoing tissue damage long after any initial trigger.
- Elevated pro-inflammatory cytokines: Signalling proteins such as TNF-alpha, IL-6, and IL-17 that drive inflammation and are found at elevated levels across most autoimmune conditions.
- Oxidative stress: Excessive free radical activity that compounds tissue damage and depletes the body's antioxidant defences.
- Mitochondrial dysfunction: Impaired cellular energy production, contributing to the fatigue that is one of the most common and debilitating features of autoimmune disease.
- Gut barrier disruption: Compromised intestinal integrity, which allows bacterial products to enter the bloodstream and further activate the immune system.
- T-cell imbalance: A shift away from regulatory immune activity toward inflammatory immune activity, sustaining the autoimmune cycle.
Conventional medicine has historically focused on symptom suppression. Research has increasingly revealed something different: that restoring immune balance, rather than simply dampening immune activity, may offer a more sustainable path for many patients