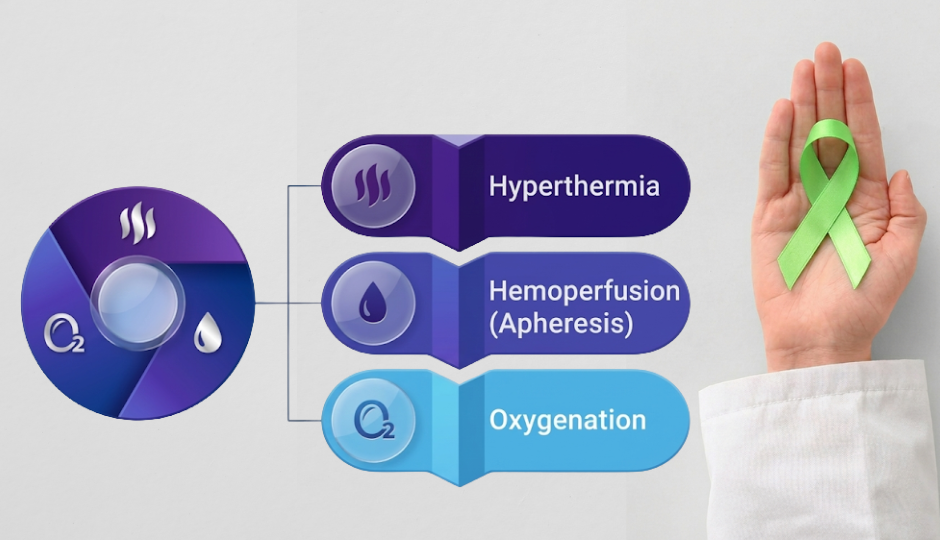
A chronic infection is one in which a pathogen persists in the body despite treatment, or in which the inflammatory and immune consequences of an infection continue long after the pathogen itself has been cleared. The distinction matters clinically because treatment strategies vary by scenario.
Standard antibiotics work well against acute infections. Chronic infections are a different problem. Several biological mechanisms allow pathogens to persist despite repeated treatment, such as:
- Biofilm formation: Bacteria construct a protective matrix around themselves that dramatically reduces antibiotic penetration and shields them from immune cells.
- Pathogen persistence: Certain organisms adopt dormant forms that are inherently resistant to antibiotic activity and can hide within tissues for extended periods.
- Systemic toxic burden: Pathogens and the inflammatory processes they trigger release toxins and metabolic byproducts that accumulate in the bloodstream, driving fatigue, neurological symptoms, and organ stress.
- Immune dysregulation: Chronic infections suppress and misdirect the immune response over time, creating persistent low-grade inflammation that damages healthy tissue even when pathogen load is reduced.
- Tissue hypoxia: Chronic infection depletes oxygen in affected tissues, creating conditions in which pathogens thrive and the body's repair mechanisms are impaired
These factors explain why chronic infections resist conventional treatment, and why an approach that operates at the level of the blood and systemic environment is clinically relevant.