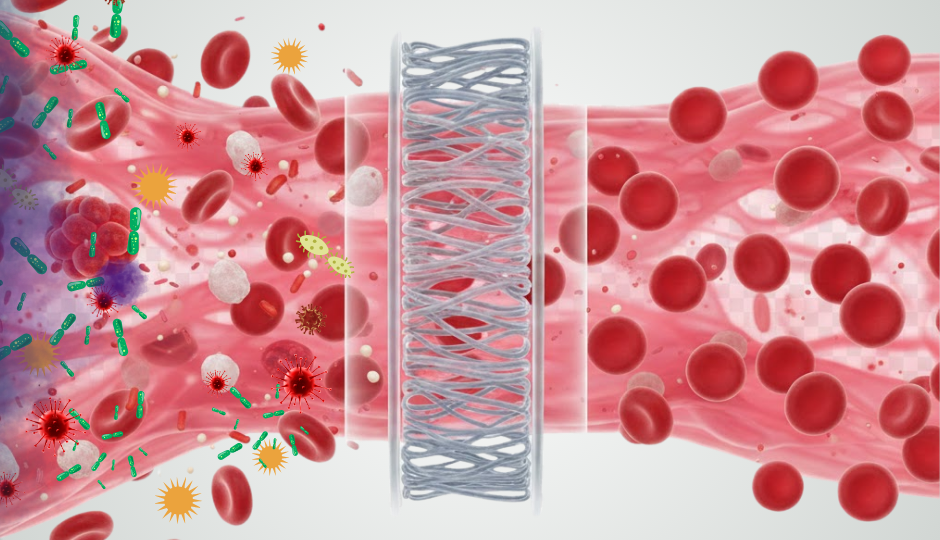
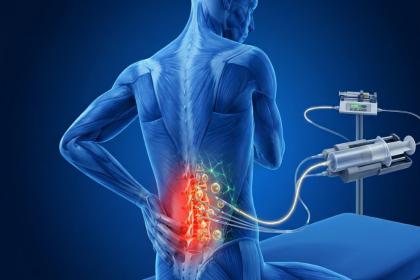
EHP® is not a single intervention. It is a combined extracorporeal procedure that integrates three distinct mechanisms: haemoperfusion, hemo-hyperthermia, and oxygenation, delivered simultaneously during a single treatment session. Blood is drawn from the patient, passed through a specialised external circuit where all three processes occur, and returned to the body.
Each component has a different function:
- Haemoperfusion passes the blood through a specialised adsorbent cartridge that selectively removes toxins, inflammatory mediators, and tumour-associated substances from the bloodstream, reducing the systemic burden that both the cancer and its treatment generate
- Hemo-hyperthermia heats the blood to a controlled range of 40°C to 42°C as it moves through the circuit. This is distinct from whole-body hyperthermia, which carries far greater physiological risk. At this temperature range, cancer cells, which are less heat-tolerant than healthy cells, are weakened and rendered more susceptible to conventional treatments such as chemotherapy and radiotherapy
- Oxygenation elevates tissue oxygen saturation substantially. Many tumour cells exploit low-oxygen environments to resist treatment and promote aggressive behaviour. Restoring oxygen availability disrupts this, supports cellular repair in surrounding healthy tissue, and promotes neovascularisation
The combination of these three processes, delivered simultaneously within a single circuit, is what distinguishes EHP® from other supportive approaches.